HOW TO AVOID COMMON PROCUREMENT MISTAKES IN CLINICS: A COMPREHENSIVE GUIDE TO STRATEGIC HEALTHCARE SUPPLY MANAGEMENT
Healthcare procurement represents one of the most critical operational functions in modern clinics, directly impacting patient care quality, operational efficiency, and financial sustainability. With healthcare costs continuing to rise and patient expectations increasing, avoiding procurement mistakes has become essential for clinic success. This comprehensive guide examines the most common procurement pitfalls and provides actionable strategies to help clinic administrators, procurement professionals, and healthcare leaders optimize their supply chain operations.

Understanding the Healthcare Procurement Landscape
Healthcare procurement encompasses the complex process of acquiring medical equipment, pharmaceuticals, supplies, and services necessary for clinical operations. Unlike procurement in other industries, healthcare purchasing involves unique challenges including regulatory compliance, patient safety requirements, and the critical nature of medical supplies where shortages can directly impact patient outcomes.
The modern healthcare procurement environment is characterized by increasing complexity, with clinics managing multiple suppliers, diverse product categories, and stringent quality requirements. According to industry research, procurement represents approximately 30-40% of a typical healthcare organization’s operational expenses, making effective procurement management crucial for financial sustainability Pandion Alliance.

The Critical Importance of Strategic Procurement
Effective procurement directly influences patient care outcomes, operational efficiency, and financial performance. Poor procurement decisions can result in supply shortages, increased costs, regulatory non-compliance, and ultimately compromised patient safety. Conversely, strategic procurement enables clinics to maintain optimal inventory levels, control costs, ensure product quality, and support clinical excellence.
Healthcare procurement’s unique characteristics include the need for specialized equipment and materials, strict regulatory compliance requirements, and the critical nature of supply availability. Unlike other industries where delays may cause inconvenience, healthcare procurement failures can be life-threatening, making error prevention paramount.
Common Procurement Mistake #1: Inadequate Needs Assessment
The Problem
One of the most fundamental mistakes in clinic procurement is failing to conduct thorough needs assessments before making purchasing decisions. This oversight leads to acquiring inappropriate equipment, over-purchasing unnecessary items, or under-purchasing critical supplies.
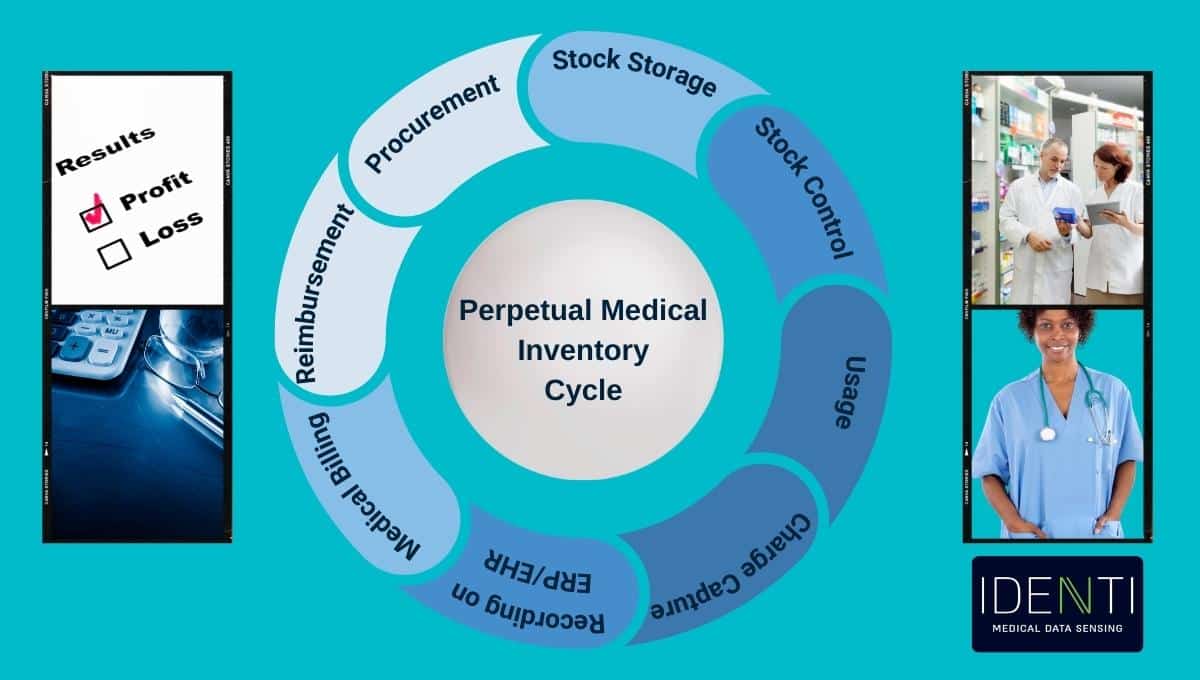
Root Causes
Inadequate needs assessment typically stems from insufficient communication between clinical staff and procurement teams, lack of standardized assessment procedures, and pressure to make quick purchasing decisions without proper evaluation.
Solutions
Implement comprehensive needs assessment protocols that involve clinical staff, department heads, and procurement professionals. Establish regular needs review meetings, develop standardized assessment forms, and create cross-functional teams to evaluate procurement requirements. Utilize data analytics to identify usage patterns and predict future needs based on historical consumption data.
Common Procurement Mistake #2: Decentralized and Disorganized Purchasing
The Problem
Many clinics suffer from fragmented procurement processes where individual departments or practitioners make independent purchasing decisions without coordination. This approach leads to missed volume discounts, duplicate purchases, and inconsistent supplier relationships.
Root Causes
Decentralized purchasing often results from lack of centralized procurement policies, insufficient communication between departments, and absence of integrated procurement systems. Individual departments may prioritize convenience over cost-effectiveness, leading to suboptimal purchasing decisions.

Solutions
Establish centralized procurement policies and procedures that govern all purchasing activities. Implement procurement software solutions that provide visibility across departments and enable coordinated purchasing decisions. Create standardized vendor catalogs and preferred supplier lists to streamline ordering processes while maintaining quality standards.
Common Procurement Mistake #3: Poor Vendor Management and Due Diligence
The Problem
Selecting vendors based solely on price without considering reputation, quality, reliability, and service capabilities represents a significant procurement risk. This approach can result in supply disruptions, quality issues, and inadequate support services.
Root Causes
Insufficient vendor evaluation processes, lack of standardized selection criteria, and pressure to minimize costs without considering total value proposition contribute to poor vendor selection decisions.

Solutions
Develop comprehensive vendor evaluation criteria that include financial stability, quality certifications, regulatory compliance, delivery performance, and customer service capabilities. Implement formal vendor qualification processes, conduct regular performance reviews, and maintain diverse supplier portfolios to mitigate risk.
Common Procurement Mistake #4: Ignoring Total Cost of Ownership
The Problem
Many clinics focus exclusively on initial purchase prices without considering long-term costs including maintenance, training, consumables, and replacement parts. This narrow focus can result in significantly higher overall costs despite lower upfront expenses.
Root Causes
Budget constraints, short-term financial planning horizons, and lack of comprehensive cost analysis capabilities contribute to inadequate total cost of ownership assessments.
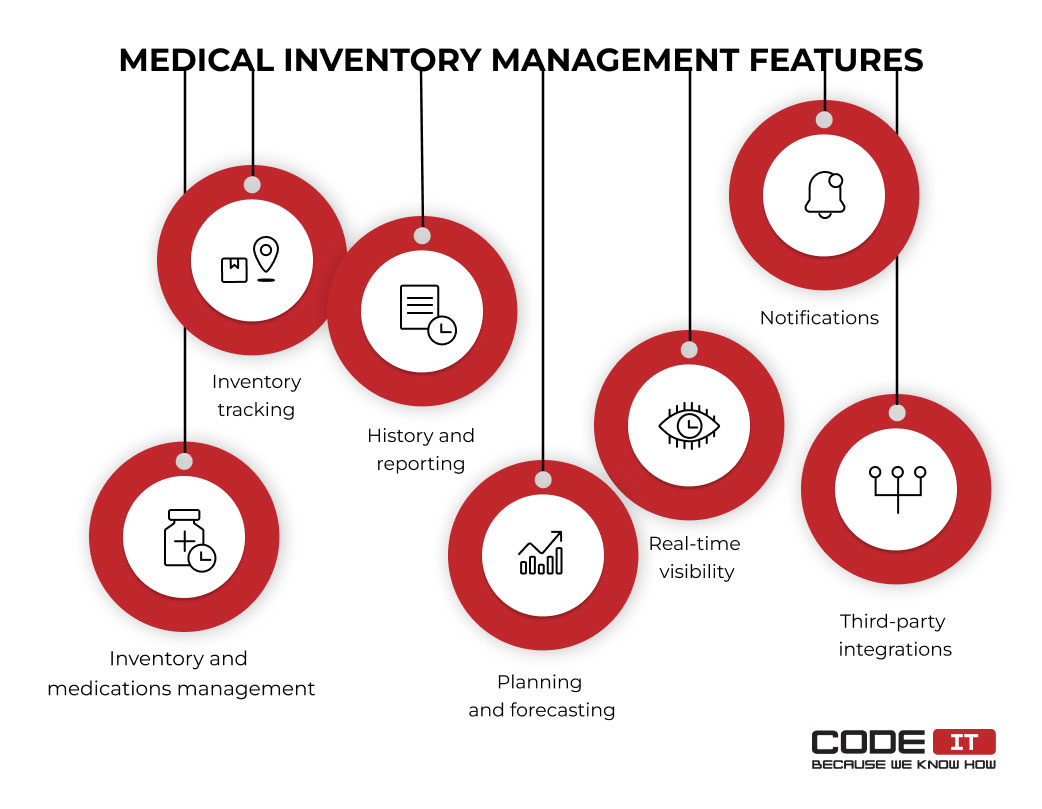
Solutions
Implement total cost of ownership analysis frameworks that evaluate all direct and indirect costs over equipment lifecycles. Include maintenance costs, training expenses, consumable requirements, and disposal costs in purchasing decisions. Develop lifecycle cost models to compare alternatives effectively.
Common Procurement Mistake #5: Inadequate Inventory Management
The Problem
Poor inventory management leads to stockouts of critical supplies, excessive carrying costs from overstocking, and waste from expired products. These issues directly impact patient care and operational efficiency.
Root Causes
Manual inventory tracking systems, lack of real-time visibility, inadequate demand forecasting, and insufficient inventory policies contribute to poor inventory management.
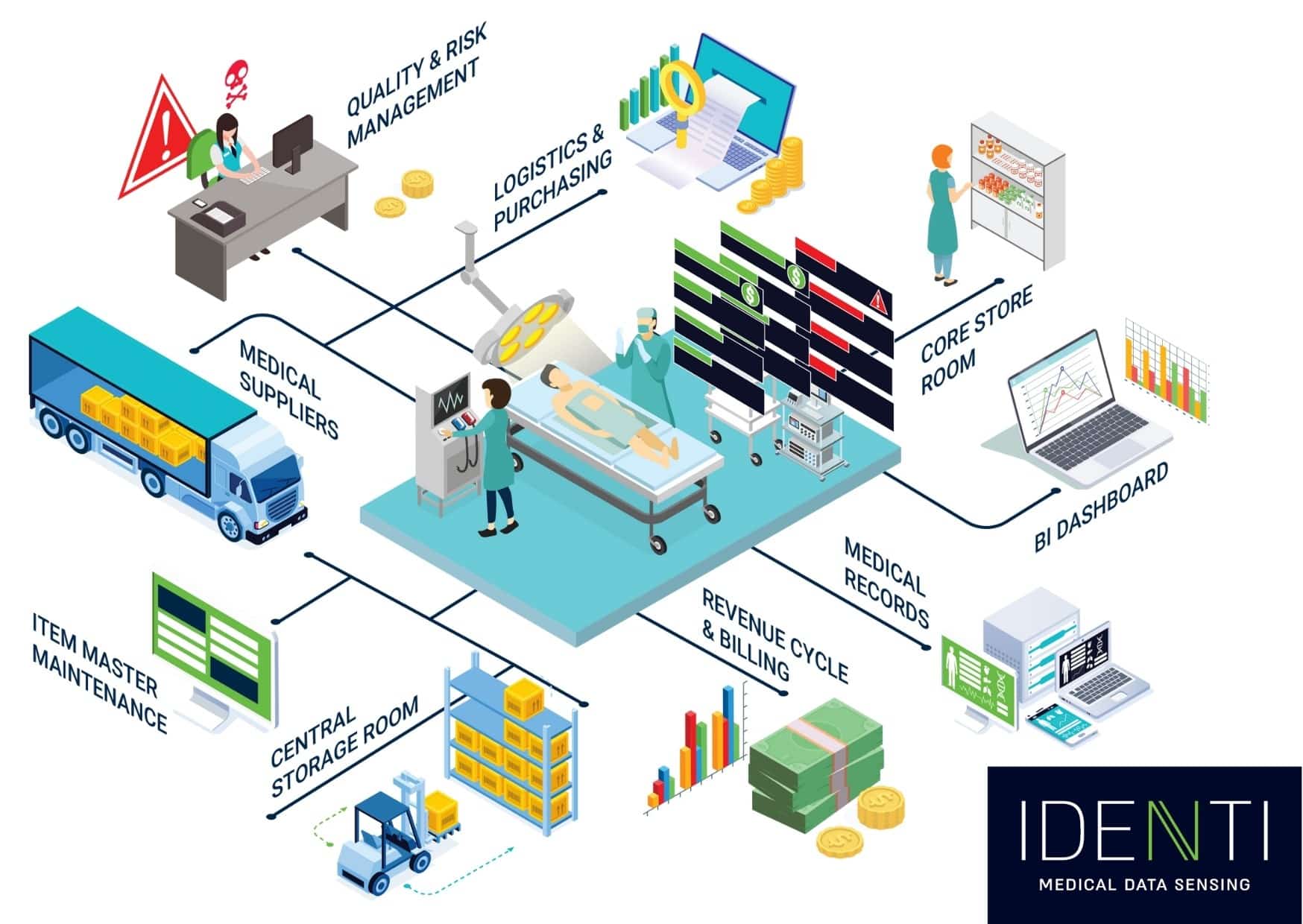
Solutions
Implement automated inventory management systems with real-time tracking capabilities. Establish appropriate inventory levels based on usage patterns, lead times, and criticality. Utilize demand forecasting tools to predict future requirements and optimize stock levels.
Common Procurement Mistake #6: Insufficient Regulatory Compliance Oversight
The Problem
Healthcare products must comply with numerous regulatory requirements including FDA approvals, safety standards, and quality certifications. Non-compliant products can result in regulatory penalties, patient safety risks, and legal liability.
Root Causes
Complex regulatory landscapes, frequent regulatory changes, and insufficient compliance monitoring systems contribute to regulatory oversight failures.
Solutions
Establish comprehensive regulatory compliance programs that track product certifications, monitor regulatory changes, and ensure supplier compliance. Implement vendor certification requirements and regular audits to verify ongoing compliance.
Common Procurement Mistake #7: Poor Contract Management
The Problem
Inadequate contract management results in unfavorable terms, missed savings opportunities, and supplier relationship issues. Many clinics fail to leverage their purchasing power effectively through strategic contracting.
Root Causes
Limited contract management expertise, decentralized contracting processes, and insufficient contract monitoring contribute to poor contract outcomes.

Solutions
Develop standardized contract templates and negotiation strategies. Implement contract management systems to track terms, performance metrics, and renewal dates. Establish cross-functional contract review teams to ensure favorable terms and conditions.
Common Procurement Mistake #8: Technology Integration Failures
The Problem
Many clinics underestimate the importance of technology integration in procurement processes, resulting in manual inefficiencies, data inconsistencies, and limited visibility into procurement activities.
Root Causes
Limited technology budgets, lack of technical expertise, and resistance to change contribute to inadequate technology adoption in procurement processes.
Solutions
Invest in integrated procurement software solutions that automate routine tasks, provide real-time visibility, and enable data-driven decision making. Ensure systems integration across departments and provide adequate training for users.
Building a Strategic Procurement Framework
Establishing Procurement Policies and Procedures
Develop comprehensive procurement policies that define roles, responsibilities, approval authorities, and standardized procedures. Ensure policies address ethical considerations, conflict of interest provisions, and compliance requirements.
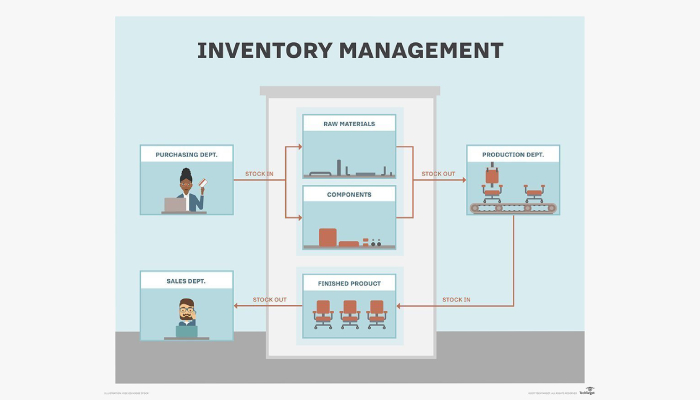
Implementing Performance Metrics and KPIs
Establish key performance indicators to measure procurement effectiveness including cost savings, supplier performance, inventory turnover, and compliance metrics. Regular monitoring and reporting enable continuous improvement and informed decision making.
Creating Cross-Functional Teams
Form procurement committees that include clinical staff, administrators, finance professionals, and quality assurance personnel to ensure comprehensive evaluation of procurement decisions and alignment with clinical needs.
Advanced Procurement Strategies
Group Purchasing Organizations (GPOs)
Leverage group purchasing organizations to access volume discounts, streamlined contracting processes, and vendor management services. GPOs can provide significant cost savings and operational efficiencies for smaller clinics.
Strategic Sourcing
Implement strategic sourcing methodologies that evaluate total value proposition rather than price alone. Consider factors such as quality, reliability, innovation, and strategic alignment in supplier selection decisions.

Supply Chain Risk Management
Develop comprehensive risk management strategies that identify potential supply chain disruptions and establish contingency plans. Consider geographic diversification, alternative suppliers, and emergency procurement procedures.
Leveraging Technology for Procurement Excellence
Automated Procurement Systems
Implement e-procurement platforms that automate routine purchasing activities, provide workflow management, and ensure policy compliance. These systems reduce manual errors, improve efficiency, and provide audit trails.
Data Analytics and Business Intelligence
Utilize data analytics to identify spending patterns, optimization opportunities, and performance trends. Business intelligence tools enable informed decision making and continuous improvement initiatives.
Integration with Clinical Systems
Ensure procurement systems integrate with electronic health records, inventory management systems, and financial systems to provide comprehensive visibility and streamline operations.
Financial Management and Cost Control
Budget Planning and Forecasting
Develop sophisticated budget planning processes that consider seasonal variations, volume changes, and capital equipment needs. Utilize historical data and predictive analytics to improve forecasting accuracy.
Spend Analysis and Cost Optimization
Conduct regular spend analysis to identify cost reduction opportunities, consolidation possibilities, and pricing optimization strategies. Monitor spending trends and benchmark against industry standards.

Value-Based Purchasing
Implement value-based purchasing strategies that consider quality, outcomes, and total cost of ownership rather than initial price alone. This approach supports better patient outcomes while controlling costs.
Quality Assurance and Risk Management
Supplier Quality Management
Establish comprehensive supplier quality management programs that include qualification processes, performance monitoring, and continuous improvement initiatives. Regular audits and assessments ensure ongoing quality compliance.
Product Standardization
Implement product standardization initiatives to reduce inventory complexity, improve purchasing efficiency, and enhance clinical workflow consistency. Standardization also enables better volume discounting and simplified training requirements.
Emergency Preparedness
Develop emergency procurement procedures and maintain strategic reserves of critical supplies. Establish relationships with emergency suppliers and create contingency plans for supply chain disruptions.
Training and Development
Staff Education and Training
Provide comprehensive training for procurement staff, clinical personnel, and administrators on procurement policies, procedures, and best practices. Regular training updates ensure awareness of regulatory changes and industry developments.
Certification and Professional Development
Encourage procurement staff to pursue professional certifications and participate in industry organizations. Continuing education ensures procurement professionals maintain current knowledge and skills.
Measuring Success and Continuous Improvement
Performance Monitoring
Implement comprehensive performance monitoring systems that track key metrics including cost savings, delivery performance, quality indicators, and customer satisfaction. Regular reporting enables timely corrective actions.
Benchmarking and Best Practices
Participate in industry benchmarking studies to compare performance against peer organizations. Identify best practices and implement improvement initiatives based on benchmark results.
Continuous Improvement Culture
Foster a continuous improvement culture that encourages innovation, efficiency enhancement, and cost reduction. Regular process reviews and improvement initiatives ensure ongoing optimization.
Conclusion: Building Procurement Excellence
Avoiding common procurement mistakes requires comprehensive planning, strategic thinking, and continuous improvement. Successful clinic procurement demands integrated approaches that consider clinical needs, financial constraints, regulatory requirements, and operational efficiency. By implementing the strategies outlined in this guide, clinics can build procurement capabilities that support excellent patient care while maintaining financial sustainability.
The key to procurement success lies in recognizing that procurement is not merely a cost center but a strategic function that directly impacts patient outcomes and organizational performance. Investment in proper procurement processes, technology, and personnel development pays dividends through improved efficiency, cost control, and patient satisfaction.
Healthcare organizations that prioritize procurement excellence position themselves for long-term success in an increasingly complex and competitive healthcare environment. By avoiding common mistakes and implementing best practices, clinics can optimize their procurement operations and focus resources on their primary mission: delivering exceptional patient care.
